As demand for retina care continues to grow and more office-based treatments are developed, retina practices are finding themselves handling higher patient volumes than ever before. This often means either finding ways to help current physicians be more productive or hiring more physicians. Both solutions create a physical space issue, and your team must find ways to add additional examination lanes, waiting space, and staff (and staff space).
At a Glance
- A practice flow assessment helps your team identify how well the current office is supporting an efficient flow, pinpoint issues, and brainstorm solutions.
- You can increase patient volume without adding space, potentially by adjusting the schedule to even out the number of physicians working at a time.
- When adding to your original footprint or converting non-patient care space into additional clinical space, look at the entire space to see how it should flow.
In this article, I discuss how your practice can get more out of what you already have and how to get the most out of a necessary renovation/expansion with little disruption to your practice flow.
THE INITIAL ASSESSMENT
Whether working with the space you have or expanding, the first step toward addressing your needs is assessing the current practice flow, space usage, and productivity.
This practice flow assessment is an operationally focused evaluation of how you are using the current space and staff and how the physicians are using their time. The goals of this exercise are to: 1) identify how well the current office is supporting an efficient and productive practice flow, 2) pinpoint issues, and 3) brainstorm solutions. You and your team should concentrate on the following:
- how the physicians are using their time (eg, look at the physicians’ weekly schedule to determine how many are in clinic at the same time);
- how long patients are waiting, whether in waiting areas, imaging, or in the examination lanes;
- the rate of patient visits per day based on the appointment template; and
- the flow of patients based on visit types.
This information is important because all decisions pertaining to the practice’s setup should be based on the best procedures that allow physicians to spend time practicing medicine, instead of lost to inefficient space, systems, or staffing models. These operational findings are then used to assess the current practice space to determine if it can be renovated or expanded to better support the practice. If not, a larger space may be required.
All too often, physicians believe the answer to eliminating wasted time in their day is to schedule more patients and have more examination lanes, but that is rarely the right approach.
Bottlenecks in practice flow are due to a disconnect in the input-throughput-output of the practice. Physicians are the output, and practice managers must know each physician’s natural rate—how many patients they can see in an hour without any delays—to determine how everything upstream (ie, input and throughput, or the patient appointment template, tech workup, imaging, front desk tasks, etc.) should be set up. Using this model, patient scheduling should be determined as follows:
- Each physician’s natural rate determines how many patients per hour should be scheduled.
- The natural rate plus the average amount of time staff requires to prepare the next patient determines how many lanes and technicians each physician needs.
- The total rate of all doctors in the office at any given time determines how many parking spaces, waiting room seats, and receptionists are needed.
Once you have completed the time study for both physicians and staff (step 2 above), you can project the time needed for each patient; if this number does not match what the physicians feel is needed, assess the processes of the appointment template flow. For example, evaluate how patients move through the clinic and how many times they are handed off from technician to technician. Are injections done in an examination lane, or is the patient moved to an injection room? Are injections grouped into an injection clinic, or are they spread throughout the day? The answers to these questions can help you adjust the patient flow of the office and, hopefully, eliminate physician delays and increase productivity without adding examination lanes.
Don’t forget to assess how long patients wait in examination lanes. Technicians only need to be one to two patients ahead of physicians, not three to four; preparing too far ahead occupies examination lanes unnecessarily and creates longer waits for patients in small, often uncomfortable rooms.
IMPLEMENTING CHANGE
Once you have a full assessment of your practice’s workflow and unmet needs, you can find ways to increase patient volume without renovating or adding space. For example, did you notice large disparities in the number of physicians in the clinic at once? If you have four physicians in the office on some days, but only two on others, adjusting the weekly schedule to even out the number of physicians working at a time (say, three) may be a better use of your space and limit examination lane bottlenecks. Changing a physician’s weekly schedule is not an easy topic to broach, but all physicians should embrace the goal of efficiency and improving patient care with the lowest possible overhead.
A Bigger Footprint
If your assessment suggests that you don’t have enough space, you may be able to address flow issues within your practice without moving offices entirely. Most practices do not have empty space just sitting around; therefore, this will require renovating to add additional space, or converting existing non-patient care space. Either way, you must find a way to transform your practice space while staying open with as little disruption to patient care as possible.
The best scenario is that you already thought of how additional space could be created when the time came. Let’s discuss Practice A as an example (Figure 1). The practice owned space adjacent to the current office; it did not need the space initially, but the master plan included expansion when necessary. This additional space could be leased and subleased until needed, or the practice could have first right of refusal from the landlord.

Figure 1. Practice A purchased space at the outset that was used as storage or subleased to the adjacent office until it was needed (A). When the practice was ready to grow, a careful renovation incorporated the new space beautifully (B).
If your practice did not plan for additional growth and your transformation needs to happen within your existing suite, the typical solution is to relocate non-patient care areas, such as administration and business office functions, to another location. During the COVID-19 pandemic, many practices moved business office functions to remote work, and that has remained a viable option for many even after the pandemic.
Although this provides more space for clinical activities, business space is rarely conveniently located to mesh into the current clinic. If you convert the back-office space into clinical space without blending it into your workflow, you risk exacerbating your flow issues.
When adding to your original footprint or converting non-patient care space into additional clinical space, look at the entire space—new and existing—to see how it should flow. The solution will probably require renovation beyond the new space, but doing so will create a much better solution.
The medical space planner and contractor will need to come up with a solution that allows the practice to stay open and minimize disruptions. The best approach is often renovating through phases. You can build out the new areas and then move portions of the practice into the new areas to free up other areas for renovation. During this process, some areas will be used differently for a short time, and temporary walls can help you separate construction zones from clinical space. Unfortunately, depending on the magnitude of the renovation, the practice may need to shut down for a day here and there. This is often done over a long weekend to minimize the disruption to patient care.
Let’s discuss Practice B as an example. Initially, the practice had space to accommodate three physicians at once but often squeezed four into the schedule (Figure 2). The practice had already moved the business office functions across the hall but had reached a point that it needed to expand again to accommodate six physicians. Thus, the practice repurposed existing space and renovated new space to create a larger overall suite that addressed both flow issues and space needs (Figure 3).
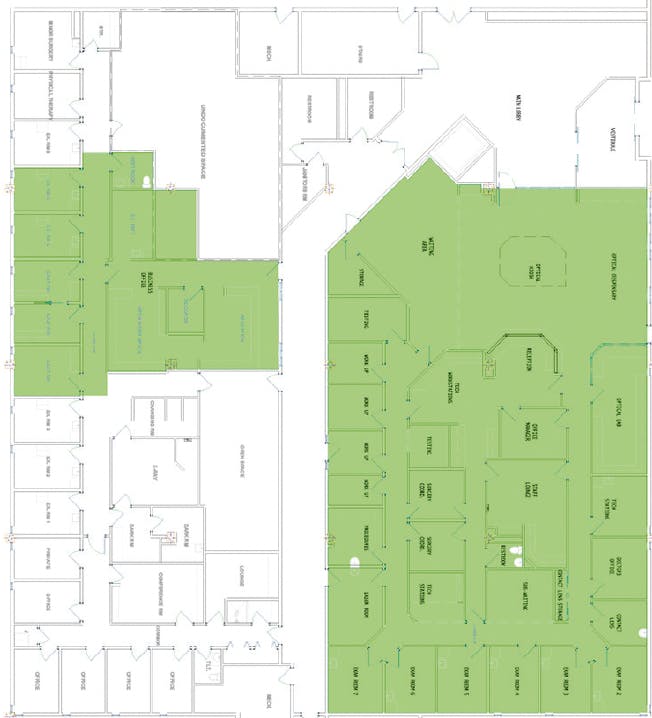
Figure 2. Practice B started with enough space to handle three physicians at a time. To squeeze in a fourth practitioner, it moved the business office functions across the hall (green).

Figure 3. Practice B used the entire floor of the building and then renovated both new and existing space to create an efficient workflow for a total of six physicians. In this solution, the general optometry patients go left, and the specialty/retina patients go right. To make the plan work, the practice took over the common hall that had initially split the practice. This flow also allowed a separation from the construction while the practice functioned normally. The practice moved into the new space and set up a temporary check in/out while the existing space was renovated.
GROW WITH CARE
Many retina practices are straining with the onslaught of patients in need of specialty care. For those who are ready to make a change, a careful renovation can make a huge difference in practice efficiency and help you better care for your patients.







