When performing vitreoretinal surgery on patients with significant mobility issues, there are certain accommodations that must be provided in the preoperative, intraoperative, and postoperative periods. In the following sections, we present a case of a patient with ankylosing spondylitis who required a modification to our typical surgical protocols; we also itemize the relevant challenges and offer suggestions for approaching similar cases.
PREOPERATIVE CONSIDERATIONS
A 68-year-old man with a 20-year history of ankylosing spondylitis, chronic ischemic cardiopathy, and moderate bronchial asthma was referred to our ophthalmology practice for poor vision in his right eye.
Due to the patient’s nuchal rigidity, we could not assess him at the slit lamp or obtain OCT images. The diagnosis and preoperative exploration were established through indirect ophthalmoscopy, owing to the observation of a sizable macular hole with white-colored deposits in its center. However, we could not ascertain its size or stage preoperatively. Keeping in mind the patient’s age and comorbidities, we decided to perform a phacovitrectomy with the insertion of an IOL and internal limiting membrane (ILM) peeling.
For the preanesthesia study, we ordered a chest x-ray (Figure 1), functional respiratory tests, and reports from pneumology, cardiology, and anesthesia specialists. Based on the results of these tests, the surgery was determined to be high risk due to many factors, including a Mallampati score of IV, poor cervical extension, poor buccal opening, thyromental distance > 6 cm, and dental prostheses.
We initially considered operating in a forced Trendelenburg position, which we attempted with the patient during the preanesthesia consultation. However, the patient did not tolerate the position well due to an increase in the venous delay of the craniofacial area; thus, the option of intervening with sedation was disregarded.
With the estimated duration of the intervention in mind, we opted for fiberoptic intubation while the patient was awake followed by use of general anesthesia.
INTRAOPERATIVE CHALLENGES
Positioning the Patient
Intubation with a fiberscope was met with considerable technical difficulty due to the need to perform it while facing the patient. With the patient’s status monitored while fully under anesthesia, he was placed into a forced Trendelenburg position (Figure 2).
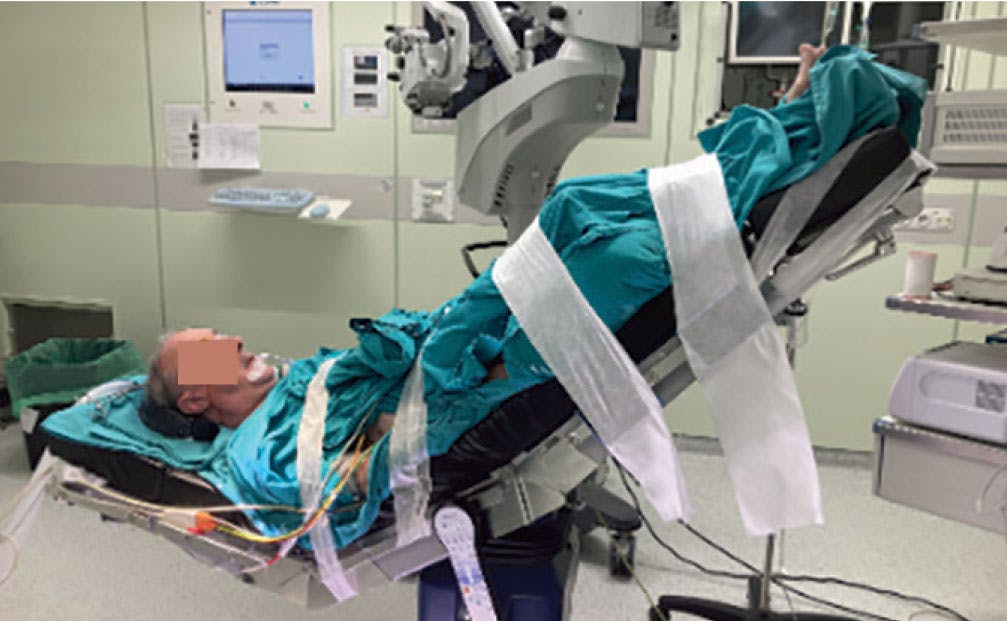
Figure 2. These photos show the patient’s final positioning for surgery after making all necessary modifications. Note his superciliary arch.
The headrest was removed from the stretcher, and an extra module was added to the end toward the patient’s feet to accommodate his neck. The idea behind this placement was to ensure the eye remained in a coaxial position with respect to the microscope and to ensure the headrest would not be too low for the surgeon. The patient was secured through several straps to prevent him from sliding down, and shoulder pads were also used to maintain the position.
The process of anesthesia and securing the patient’s position required approximately 1 hour and 15 minutes.
Positioning the Surgeon
At this point, the main surgeon placed himself laterally to have suitable access to the eye, as the patient’s head and superciliary arch did not allow for any other approach. Because of the stretcher modifications, the surgeon moved the pedals in an uncomfortable position. Moreover, because of the patient’s position, the surgical microscope kept making contact with the superior area of the superciliary arch, so it was impossible to see the entire superior hemiretina.
After performing 23-gauge posterior vitrectomy and ILM staining, a contact lens was used to achieve a clearer image of the posterior pole. Because the lens kept moving downward, the trocars were switched to the 7 clock hour position (right hand), inferior nasal (infusion), and superior temporal (endocular light).
During the surgery, a posterior vitreous detachment was found, and it was possible to diagnose the patient with a stage 4 macular hole based on the Gass classification and epiretinal proliferation. Due to the inability to perform intraoperative OCT, no images were taken during the surgery.
When peeling the ILM, the superior zone of the contact lens made contact with the superciliary arch, so the surgeon’s assistant had to cut one of lens haptics to make it more horizontal.
After completing the vitrectomy with 25% SF6, the nylon 10/0 stitch was removed because, due to the patient’s short chin-sternum distance, it would be impossible to remove it at the slit lamp.
POSTOPERATIVE CARE
It is essential to schedule regular postoperative examinations to support visual and anatomic rehabilitation and monitor for complications. In this case, postoperative assessment was also conditioned to the patient’s nuchal rigidity. In the follow-up visits, we were able to assess his visual acuity and IOP using a Perkins Mk3 tonometer (Haag-Streit) and obtain fundus imaging with an indirect ophthalmoscope. Only during one visit could we obtain a postoperative OCT image, which confirmed the macular hole closure (Figure 3).
To instill eye drops at home, the patient had to lay face up each time for the caregiver to properly administer them.
MEET THE PATIENT WHERE THEY ARE
When planning for a vitreoretinal surgery, we must assess each patient’s characteristics, surgical requirements, and postoperative care regimen. Only by considering all these factors can we choose a more customized—and less aggressive—option with the patient’s wellbeing in mind.














_1773249222.png?auto=compress,format&w=75)












