AT A GLANCE
- Gene therapy offers a promising avenue for long-term—and potentially curative—interventions for wet AMD and geographic atrophy (GA).
- At least six gene therapies are under investigation for the treatment of wet AMD with intravitreal, subretinal, and suprachoroidal delivery methods. Early data suggest some of them could decrease the annualized injection rate by 80% or more.
- Several companies are in the early phases of exploring gene therapy for GA. Preliminary results show promise, with a slowing of GA lesion growth rates for some drug candidates.
Unlike current treatment approaches for AMD (Figures 1 and 2), which focus on managing symptoms, gene therapy offers a promising avenue for long-term—and potentially curative—interventions. Here, we provide an overview of the latest advances in the field (Table).
GENE THERAPY CANDIDATES FOR WET AMD
ABBV-RGX-314 (Regenxbio/Abbvie) uses an AAV vector to deliver a gene encoding an anti-VEGF antibody fragment similar to ranibizumab.1 The phase 2 AAVIATE trial (NCT04514653) is studying suprachoroidal ABBV-RGX-314 compared with ranibizumab (Lucentis, Genentech/Roche). Interim 6-month results in 115 patients across three dose levels indicated no serious adverse events. In patients treated at the highest dose level, the therapy has resulted in an 80% decrease in the annualized injection rate and 50% of patients remaining injection-free. Additionally, no cases of intraocular inflammation were observed with a short course of prophylactic topical steroid eye drops.2 An ongoing observational trial (NCT05210803) is following patients for 5 years to assess long-term safety and efficacy.
The phase 3 ASCENT clinical trial (NCT05407636) and the phase 2/3 ATMOSPHERE (NCT04704921) trial are assessing the administration of ABBV-RGX-314 via subretinal delivery compared with 2 mg aflibercept (Eylea, Regeneron) and ranibizumab, respectively. A long-term study (NCT03999801) is following participants for up to 5 years after a single subretinal administration of ABBV-RGX-314.
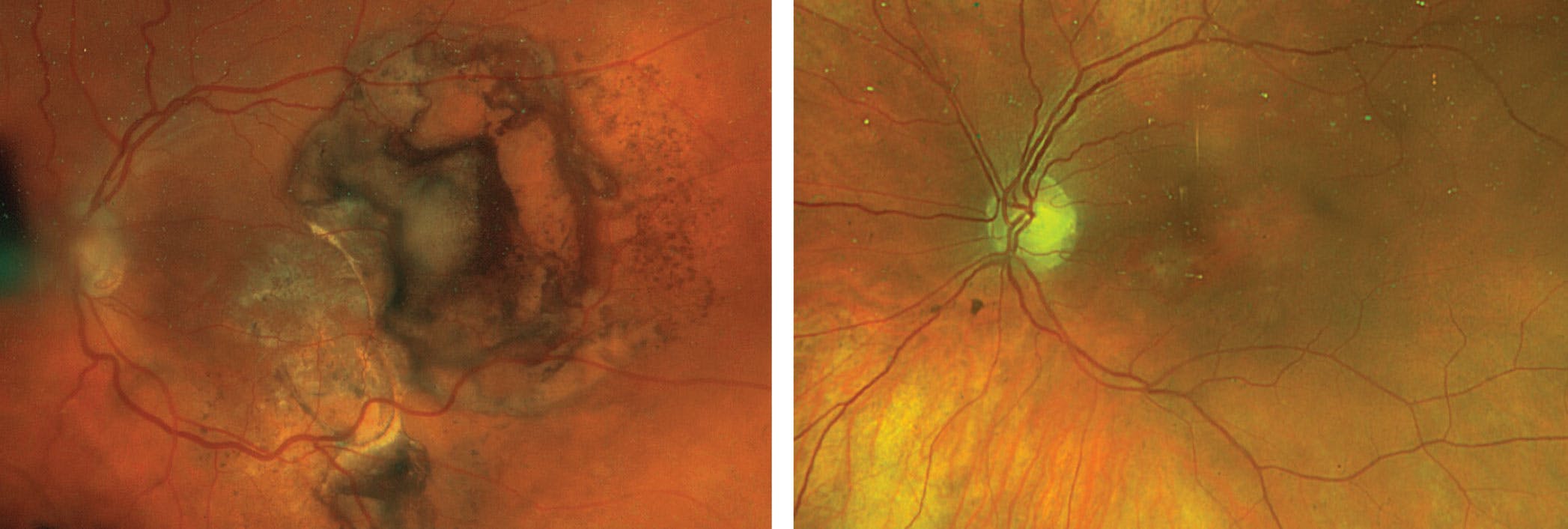
Figure 1. Gene therapies under investigation for wet AMD may one day allow patients such as these to have a one-and-done treatment.
Ixo-vec (ixoberogene soroparvovec, Adverum Biotechnologies) employs an AAV capsid, AAV.7m8, to intravitreally deliver the genetic code for aflibercept, enabling transduced retinal cells to continuously produce therapeutic levels of aflibercept. Preliminary 4-year data from the ongoing OPTIC extension study (NCT04645212) show an 86% reduction in annualized anti-VEGF injections compared with baseline. Nearly half of the participants remained injection-free, and 78% of those who were injection-free after the first year maintained that status through year 4.3
Preliminary results from the phase 2 LUNA trial (NCT05536973) show that ixo-vec reduced the need for anti-VEGF injections by 88% to 92% from baseline in 60 patients across two dose cohorts, 6E10 vg/eye and 2E11 vg/eye, respectively. At the two tested doses, 1-year injection-free rates were 54% and 69%, respectively.3 At 52 weeks, with prophylactic topical steroids, no inflammation was observed in patients receiving the low dose of ixo-vec.3 The phase 3 ARTEMIS study (NCT06856577) is enrolling 284 patients in a double-masked, randomized trial comparing ixo-vec (6E10 vg/eye) with 2 mg aflibercept.4

Figure 2. Patients with dry AMD, such as this one, now have FDA-approved treatment options and the promise of gene therapies that are currently under investigation.
4D-150 (4D Molecular Therapeutics) delivers aflibercept and a VEGF inhibitory miRNA through intravitreal injection of an AAV variant.5 In the phase 1/2 PRISM trial (NCT05197270), participants are administered either high- or low-dose gene therapy, while the control group receives bimonthly aflibercept injections. An interim analysis at 24 weeks revealed a more than 80% reduction in injection frequency across both treatment groups.6 Visual acuity remained stable in both groups, and no significant adverse events were reported.6 The company is recruiting for the 4FRONT-1 phase 3 trial (NCT06864988).
KH631 (Chengdu Origen Biotechnology) uses an AAV vector to deliver a gene encoding a VEGF receptor fusion protein, which binds to VEGF.7 In preclinical studies, KH631 demonstrated prolonged retention of the therapeutic protein in the retina and effectively prevented disease progression in wet AMD models.7 Phase 1 (NCT05657301) and phase 1/2 (NCT05672121) clinical trials are evaluating its safety and efficacy in wet AMD.
In addition, Chengdu Origen Biotechnology/Vanotech recently announced the first patient with wet AMD dosed in a phase 1 trial (NCT06825858) for KH658, another recombinant AAV vector that encodes a VEGF receptor fusion protein that is delivered into the suprachroidal space.8
FT-003 (Frontera Therapeutics) is an AAV gene expression system designed to stimulate retina cells to produce a humanized recombinant fusion protein similar to aflibercept.9 Phase 1 (NCT05611424) and phase 1/2 (NCT06492863) clinical trials are assessing its safety and efficacy in wet AMD.
HG202 (HuidaGene Therapeutics) is an RNA-editing treatment using the CRISPR/Cas13 system, delivered via a single AAV vector. The therapy is designed to reduce VEGF expression and prevent the development of choroidal neovascularization (CNV) in AMD. Preclinical studies showed an 87% reduction in CNV area, which surpasses current anti-VEGF treatments.10 Two ongoing phase 1 trials—SIGHT-I (NCT06031727) and BRIGHT (NCT06623279)—are assessing safety, tolerability, and efficacy at different doses. Initial data from the SIGHT-I trial indicated that a patient with a history of non-responsiveness to anti-VEGF injections showed significant improvement in retinal fluid, central retinal thickness, and visual acuity after a low-dose injection, with no adverse events or dose-limiting toxicity observed.11
EXG102-031 (Exegenesis Bio) is an AAV vector expressing a fusion protein that binds all four subtypes of VEGF and Ang-2 delivered subretinally. EXG202 (Exegenesis Bio) uses the same fusion protein-expressing transgene but is packaged in an ocular-specific capsid that enables a three- to five-fold increase in transduction efficiency in retinal cells, allowing administration via intravitreal injection.12 Both EXG102-031 and EXG202 are in phase 1 trials (NCT05903794 and NCT06888492, respectively).
GENE THERAPY CANDIDATES FOR GEOGRAPHIC ATROPHY
JNJ-1887 (JNJ-81201887/AAVCAGsCD59, Janssen) employs an AAV vector to enhance the expression of soluble CD59, an antiinflammatory protein that inhibits the formation of the membrane attack complex in the complement pathway.13 JNJ-1887 is delivered via a single intravitreal injection. The phase 1 study demonstrated that the gene therapy was well-tolerated across all dose levels in 17 patients, with no significant safety concerns. Notably, patients in the high-dose cohort exhibited a continuous decline in geographic atrophy (GA) lesion growth rates over 24 months.14 Janssen initiated a phase 2 clinical trial (NCT05811351) to assess the change in GA lesion growth in eyes treated with JNJ-1887 compared with sham. Additionally, a long-term extension study (NCT06635148) is underway to monitor the drug’s sustained effects and safety.
OCU410 (AAV5-hRORA, Ocugen) is designed to restore the expression of the RORA gene, which is involved in lipid metabolism and oxidative stress regulation.15 Early results from the phase 1 portion of the phase 1/2 clinical trial (NCT06018558), which includes nine participants with GA across three dosage levels, reported no serious side effects at 6 months. The treated eyes exhibited a 21.4% reduction in lesion growth compared with untreated eyes.16
GENE THERAPY DEFINED
- Gene replacement therapy introduces a functional gene copy to compensate for a defective one. It requires knowledge of the specific genetic mutation and is less effective for polygenic diseases such as AMD.1
- Gene silencing uses siRNAs or miRNAs to degrade specific mRNAs, preventing the production of harmful proteins.
- Gene editing uses CRISPR/Cas9 to directly modify DNA mutations or reduce the expression of mutated proteins.
- Modifier gene therapy regulates upstream or downstream genes that affect the expression of the malfunctioning gene.
- The ocular “biofactory” delivers genes encoding therapeutic agents directly to ocular cells, enabling them to produce these agents locally, reducing the need for intraocular injections.
- Neuroprotective gene therapy delivers factors such as pigment epithelium-derived factor (PEDF) to prevent retinal cell degeneration. In an AMD mouse model, delivery of PEDF with miRNAs effectively reduces choroidal neovascularization.2
- Optogenetics introduces light-sensitive opsins, such as melanopsin, into retinal cells to treat photoreceptor degeneration, showing promising efficacy in preclinical studies.3
1. Drag S, Dotiwala F, Upadhyay AK. Gene therapy for retinal degenerative diseases: progress, challenges, and future directions. Invest Ophthalmol Vis Sci. 2023;64(7):39.
2. Askou AL, Alsing S, Benckendorff JNE, et al. Suppression of choroidal neovascularization by AAV-based dual-acting antiangiogenic gene therapy. Mol Ther Nucleic Acids. 2019;16:38-50.
3. Prosseda PP, Tran M, Kowal T, Wang B, Sun Y. Advances in ophthalmic optogenetics: approaches and applications. Biomolecules. 2022;12(2):269.
BETTER VISION, FEWER TREATMENTS
There is a wealth of promising therapies in development for both wet and dry AMD. As research pushes forward, treatments for AMD could soon feature leading options that employ a multifaceted approach using various delivery techniques—all of which aim to preserve patients’ vision and extend treatment duration.
1. Liu Y, Fortmann SD, Shen J, et al. AAV8-antiVEGFfab ocular gene transfer for neovascular age-related macular degeneration. Mol Ther. 2018;26(2):542-549.
2. Regenxbio announces positive interim data from phase II AAVIATE trial of ABBV-RGX-314 for the treatment of wet AMD using suprachoroidal delivery [press release]. PR Newswire. January 16, 2024. Accessed February 18, 2025. tinyurl.com/525kcdbj
3. Adverum Biotechnologies announces positive 52-Week LUNA and 4-Year OPTIC results, and provides key pivotal program design elements [press release]. Adverum Biotechnologies. November 18, 2024. Accessed February 18, 2025. tinyurl.com/mtrzrahb
4. Adverum Biotechnologies initiates ARTEMIS phase 3 study evaluating ixo-vec for wet AMD [press release]. Adverum Biotechnologies. March 3, 2025. Accessed March 6, 2025. tinyurl.com/2fucebun
5. Calton MA, Croze RH, Burns C, et al. Design and characterization of a novel intravitreal dual-transgene genetic medicine for neovascular retinopathies. Invest Ophthalmol Vis Sci. 2024;65(14):1.
6. 4DMT highlights robust and durable clinical activity for 4D-150 and design of 4FRONT phase 3 program at 4D-150 wet AMD development day [press release]. 4D Molecular Therapeutics. September 18, 2024. Accessed February 18, 2025. tinyurl.com/5n96hv4e
7. Ke X, Jiang H, Li Q, et al. Preclinical evaluation of KH631, a novel rAAV8 gene therapy product for neovascular age-related macular degeneration. Mol Ther. 2023;31(11):3308-3321.
8. Chengdu Origen and Vanotech announce first patient dosed inpPhase 1 trial of gene therapy for wet AMD [press release]. Eyewire+. May 2, 2025. Accessed May 6, 2025. bit.ly/4jBXPze
9. Frontera receives FDA clearance for FT-003 phase 2 IND in neovascular age-related macular degeneration [press release]. Frontera Therapeutics. November 11, 2024. Accessed February 18, 2025. tinyurl.com/578days5
10. HuidaGene Therapeutics receives the first-ever FDA clearance of CRISPR/Cas13 RNA-editing HG202 for macular degeneration [press release]. HuidaGene Therapeutics. November 4, 2024. February 18, 2025. tinyurl.com/3hyr3jcs
11. Luk A, Xing D, Liu B, et al. World’s first CRISPR/RNA-targeting therapy (HG202) for patients with neovascular age-related macular degeneration. Invest Ophthalmol Vis Sci. 2024;65(7):4357-4357.
12. US FDA grants orphan drug designation to EXG110, a novel gene therapy for Fabry disease [press release]. BusinessWire. December 3, 2024. Accessed April 2, 2025. bit.ly/3RtUcPs
13. Tan LX, Toops KA, Lakkaraju A. Protective responses to sublytic complement in the retinal pigment epithelium. Proceedings of the National Academy of Sciences. 2016;113(31):8789-8794.
14. Heier JS, Cohen MN, Chao DL, et al. Phase 1 study of JNJ-81201887 gene therapy in geographic atrophy secondary to age-related macular degeneration. Ophthalmology. 2024;131(12):1377-1388.
15. Silveira AC, Morrison MA, Ji F, et al. Convergence of linkage, gene expression and association data demonstrates the influence of the RAR-related orphan receptor alpha (RORA) gene on neovascular AMD: a systems biology based approach. Vision Research. 2010;50(7):698-715.
16. Ocugen reports positive preliminary data from OCU410 trial for geographic atrophy [press release]. Eyewire+. November 19, 2024. Accessed February 18, 2025. tinyurl.com/h4j7t2zt










-1_1748961738.jpg?auto=compress,format&w=70)







_1773249222.png?auto=compress,format&w=75)












